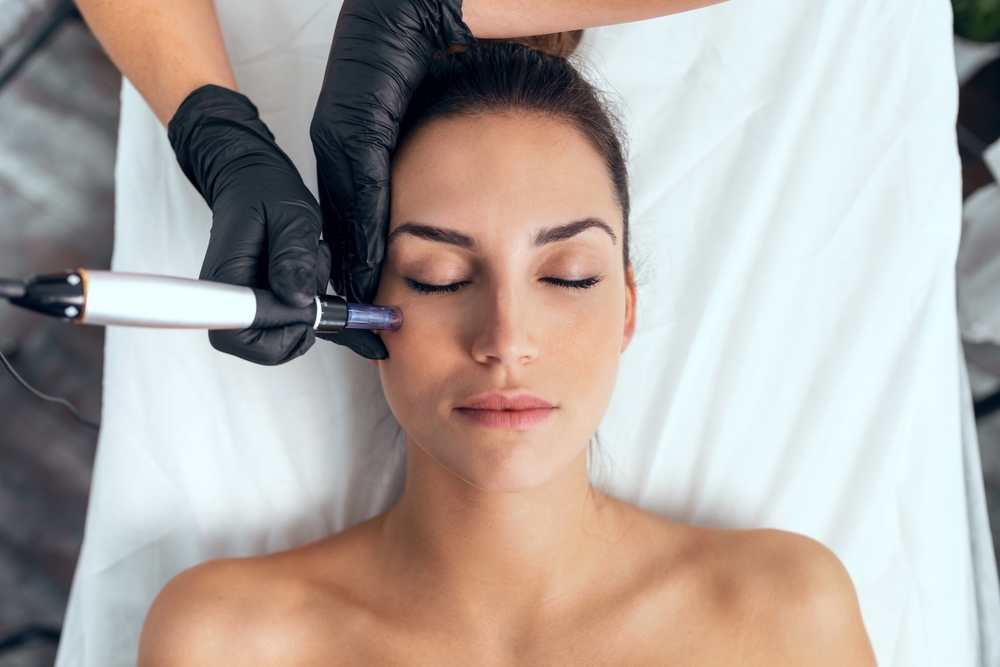
Psoriasis is a chronic, immune-mediated skin condition that requires knowledgeable medical management. Dermatologists are the primary specialists equipped to diagnose and manage this complex disease. They receive specific medical training to evaluate skin changes, interpret symptoms, and develop targeted management strategies. Through consultation with a dermatology specialist, patients can receive an accurate diagnosis and access therapeutic options tailored to their specific condition.
What Is Psoriasis?
Psoriasis is an autoimmune disease that causes skin cells to build up rapidly on the surface of the skin. This rapid cell turnover results in thick, scaly, and inflamed patches. The presentation varies significantly, depending on the specific type of psoriasis a patient develops.
Plaque psoriasis is the most common form, characterized by raised, red, inflamed skin covered with scales. These plaques frequently appear on the elbows, knees, scalp, and back, and they may be itchy or raw from scratching. Guttate psoriasis, often seen in children, typically emerges following a bacterial infection like strep throat. It presents as small, teardrop-shaped lesions on the torso and limbs. Nail psoriasis affects the fingernails and toenails, leading to pitting, abnormal nail growth, discoloration, or separation from the nail bed. Many individuals with psoriasis also develop a painful form of joint inflammation called psoriatic arthritis, which causes swollen and stiff joints alongside skin symptoms.
What Causes It?
Research indicates that psoriasis arises from a combination of genetic predispositions and immune system factors. The immune system mistakenly triggers an overproduction of new skin cells, and a family history of the disease significantly increases a person’s likelihood of developing the condition. While the root cause is genetic and immunological, various environmental factors can trigger the onset or exacerbation of symptoms.
Infections frequently precede flare-ups. Severe psychological stress is also often correlated with worsened skin symptoms. Weather changes, especially cold and dry conditions, may also aggravate the skin. Certain medications, including some for high blood pressure, can precipitate an outbreak. Skin injuries may lead to new lesions at the injury site. Lifestyle factors like smoking are also associated with increased disease severity. Identifying personal triggers is a key part of managing the condition and minimizing flare-ups.
How Is It Treated?
Dermatology provides a structured approach to managing psoriasis symptoms, with the goals of slowing skin cell growth and removing scales. A dermatologist evaluates the disease severity, the specific type of psoriasis, and the patient’s medical history before recommending a course of action. Topical treatments are often a first-line therapy for mild to moderate cases. Dermatologists prescribe topical corticosteroids and retinoids to be applied directly to the affected site. Applying soothing ointments may also be recommended to minimize itching at home.
For more extensive or persistent cases, light therapy can be utilized. This method involves exposing the skin to controlled amounts of ultraviolet light under medical supervision. In situations involving moderate to severe symptoms, dermatologists may prescribe systemic medications. These treatments, which include oral and injectable options, work throughout the body to address the underlying immune response. Dermatologists monitor patients on these therapies to manage potential side effects and adjust treatment as needed.
Seeking Professional Dermatology Services
Dermatologists provide comprehensive support to improve a patient’s approach to managing psoriasis. A primary objective of professional care is trigger identification and avoidance, which helps minimize the frequency and severity of flare-ups. Specialists educate patients on proper skincare routines, such as using specific moisturizers that complement medical therapies and prevent further skin irritation. Seeking professional care provides a structured plan for managing symptoms effectively and maintaining long-term skin health.
- Purchasing a Home in Danville, California: A Comprehensive Guide
- Streamlining Commercial Construction Projects with Modern Technology
- Transforming Your Bathroom: The Benefits of Converting a Tub to a Walk-In Shower
- The Importance of Early Detection in Chronic Venous Insufficiency
- Understanding the Microneedling Process and Its Benefits